IMAGE OF THE WEEK 2013
WEEK 17
CHRONIC
PANCREATITIS
|
 |
 |
|
|
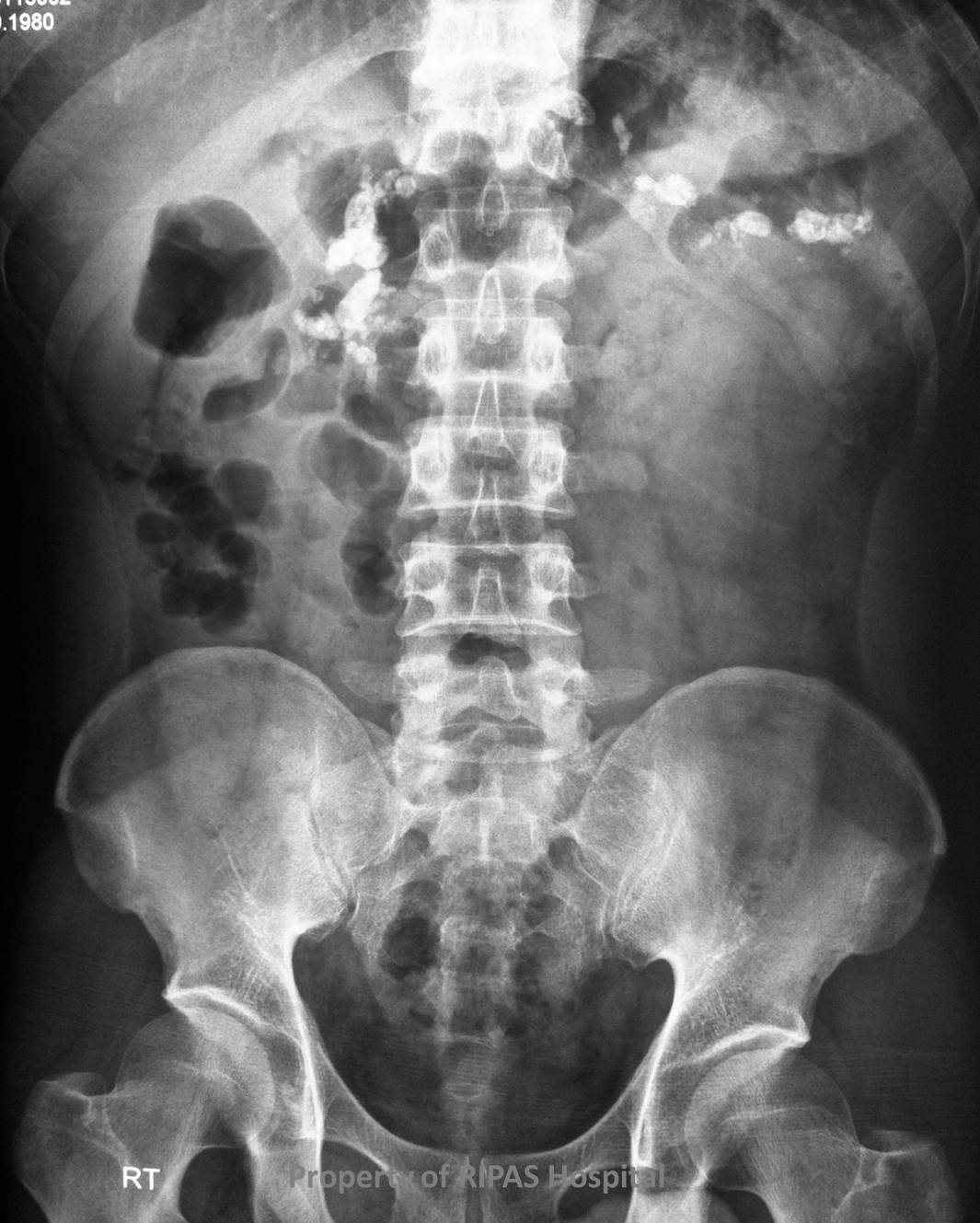
Figure 1a: Plain abdominal radiograph showing coarse
calcification along the line of the whole pancreas with osteomalacia of
the bones.
(Click on image to
enlarge) |
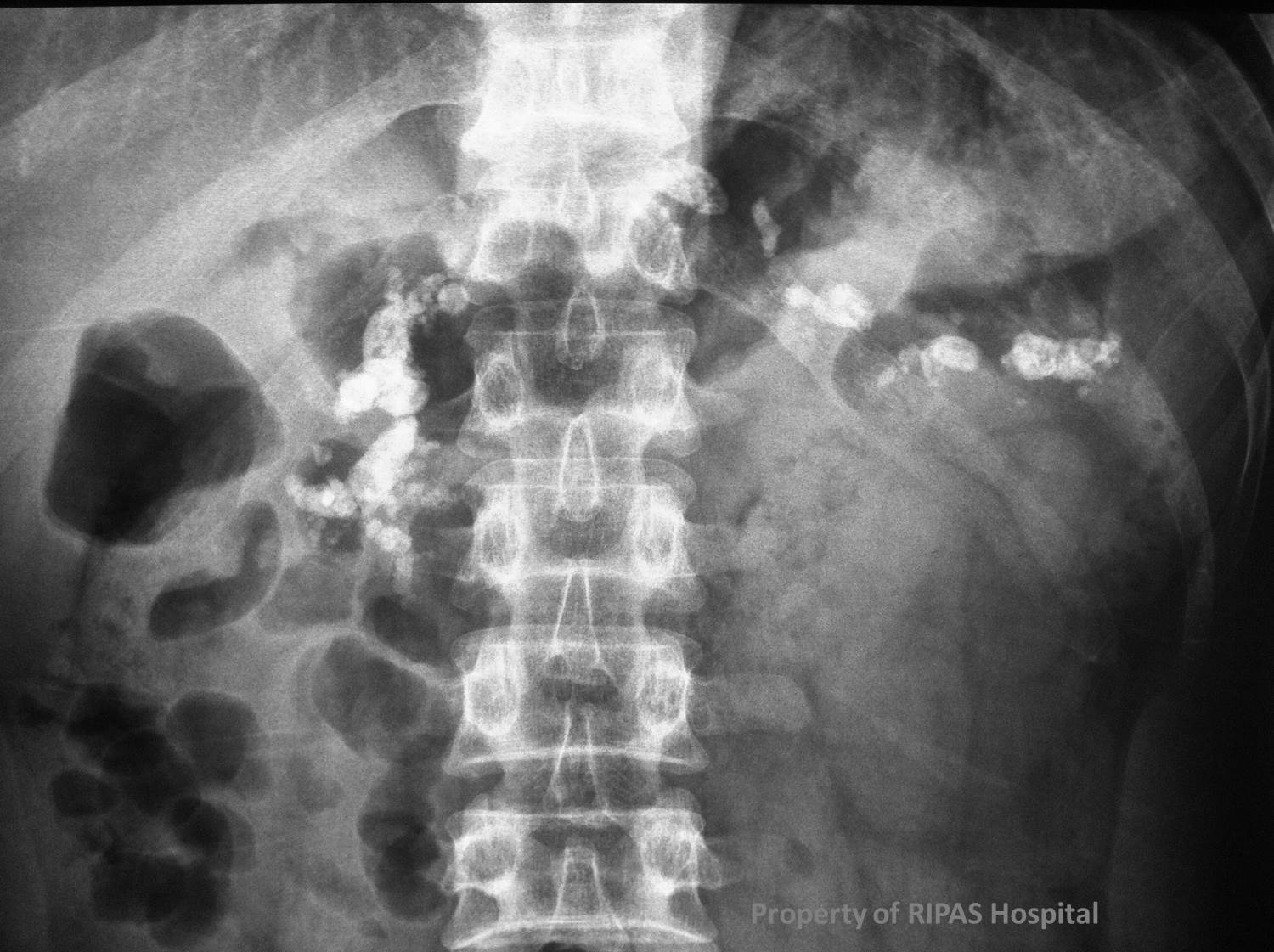
Figure 1b: Plain abdominal radiograph with
magnification of the calcified pancreas.
(Click on image to
enlarge) |
|
|
|
|
|
Chronic
pancreatitis is a condition characterized by repeated pancreatic inflammation
leading to progressive pancreatic damage and fibrosis with eventual impairment
of both exocrine and endocrine functions of the pancreas.
The
most common aetiology in the western societies is alcohol abuse. In Brunei,
gallstones are the most common aetiology, although the condition of chronic
pancreatitis is uncommon. Acute pancreatitis and chronic pancreatitis are
assumed to be different disease processes and most cases of acute pancreatitis
do not result in chronic disease.
Chronic
pancreatits can be classified into 3 types:
·
Chronic
calcifying pancreatitis – associated with alcoholism.
·
Chronic
obstructive pancreatitis – periductal fibrosis and ductal dilatation.
·
Chronic
inflammatory pancreatitis
Imaging
plays an important role in the diagnosis and management of chronic pancreatitis.
Plain abdominal radiographs show pancreatic calcification in 25-59% of patients
and is pathognomonic of chronic pancreatitis (Figure 1a and b). The coarse
calcification occurs along the distribution of the pancreas. There is also
associated osteomalacia in the spine, pelvic bones and lower limb long bones
secondary to malabsorption. CT is useful in differentiating chronic pancreatitis
from pancreatic carcinoma. The use of secretin with MR cholangiopancreatography
can be use to demonstrate pancreatic exocrine reserve.
Treatment of uncomplicated chronic pancreatitis is usually symptomatic relief of
pain, malabsorption and resulting diabetes. Minimally invasive therapy and
surgery are generally reserved for complications such as pseudocysts, abscess
and malignancy.
Images contributed by
Dr Ian Bickle, Department of Radiology,RIPAS Hospital
Text contributed by Mr
William Chong, Department of Surgery, RIPAS Hospital
All
images are copyrighted and property of RIPAS Hospital.


